Tongue ties and infant feeding challenges
Disclaimer: This information is not medical advice and should never replace the recommendations provided by your health care provider or International Board Certified Lactation Consultant (IBCLC).
If you and your baby are having a hard time with breast/chest feeding, you may be wondering “could my baby have a tongue tie?” Maybe a friend or family member suggested this to you, or through your own research you came across information that sounds exactly like what you and your baby are experiencing.
Definition of a tongue tie
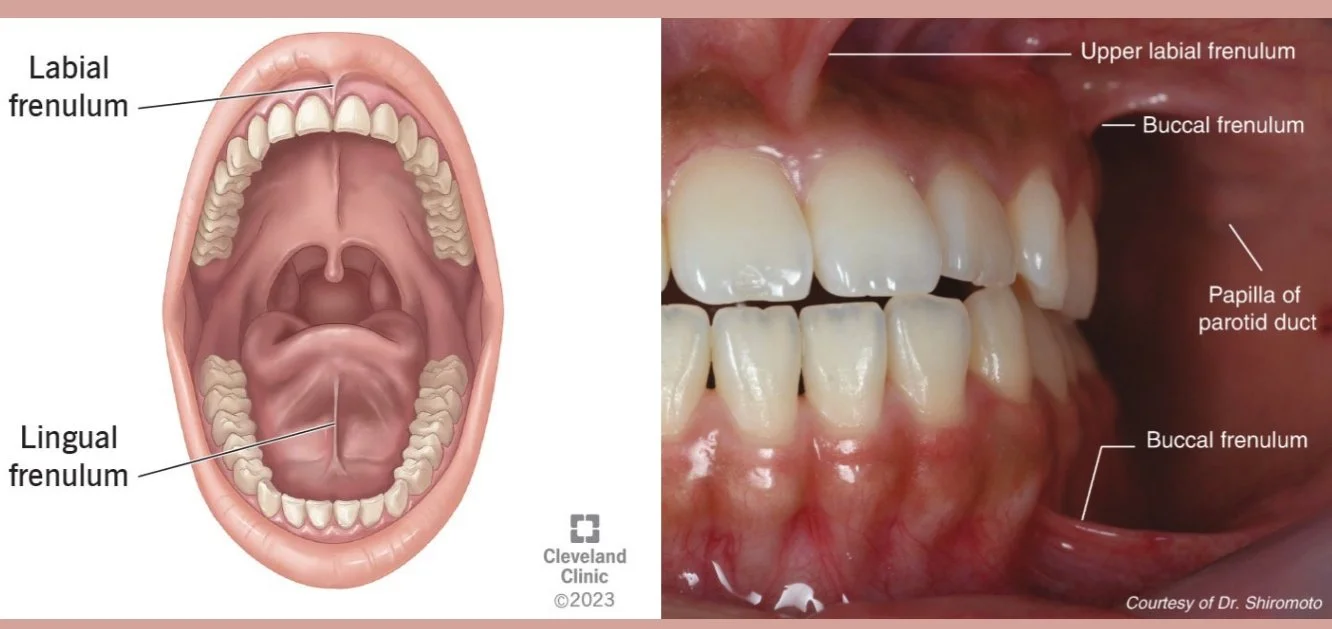
The technical term for a tongue tie is ankyloglossia. The small piece of tissue under your tongue is called a “frenulum”. Frenulum, or frenum, are small pieces of connective tissue that join two structures in our mouths. We have frenulum that connects our lips to our gums, and our tongue to our mouth. We need this support in our mouths for eating, drinking, breathing, and speech. If these tissues are really tight, or too short, it can make breastfeeding for babies really difficult.
Labial, lingual, and buccal frenum
How a tongue tie is diagnosed
Only a doctor, nurse practitioner, or dentist can diagnose a tongue tie. This can be challenging because healthcare providers need to be confident in their breastfeeding knowledge. Sometimes the common signs and symptoms of a tongue tie can be similar to other conditions. Researchers are learning more about how tongue ties can cause issues with breastfeeding, but we still need more research. At this time, there is no “gold standard” tool that providers can use to help guide them in diagnosing a tongue tie. To learn more about what healthcare providers know about tongue tie, the Canadian Pediatric Society has a Position Statement about ankyloglossia and breastfeeding.
Common signs and symptoms of a tongue tie
The most common first sign of a tongue tie is not being able to get a “good latch”. The Canadian Breastfeeding Foundation provides a step-by-step process of how to position your baby so that they achieve a “good latch” at the breast. Have a look at the image below of this older baby breastfeeding:
Visual of a “good latch”
Other common signs that may be related to a tongue tie:
Parents: painful feedings, nipple damage or wounds, flat/creases or lipstick shaped nipple after feeding, frequent blocked ducts or recurring mastitis, low milk supply, early weaning from breastfeeding.
Babies 0 to 6 months: poor latch, not able to stay latched, poor suction, clicking sounds while nursing, biting or chewing the nipple, lip blisters, slow or no milk transfer, irritability or colic, slow weight gain, gets tired quickly while nursing
Babies 6+ months: trouble with starting solids, unable to drink from a cup, speech challenges, dental concerns (teeth crowding, gingivitis, cavities)
What the research says about lip ties and cheek ties
Lip tie or “labial tie” and cheek tie or “buccal tie” have also gained a lot of attention and are often discussed in relation to breastfeeding challenges. Many parents are concerned that when their baby is breastfeeding that their lips are not “flanged” out which means they do not have a good latch. However, if you are not experiencing pain while breastfeeding, and your baby is able to drink from the breast, this is more important than what the latch looks like from the outside. The Academy of Breastfeeding Medicine , the American Academy of Otolaryngology and other researchers have not found that lip or cheek ties will impact breastfeeding.
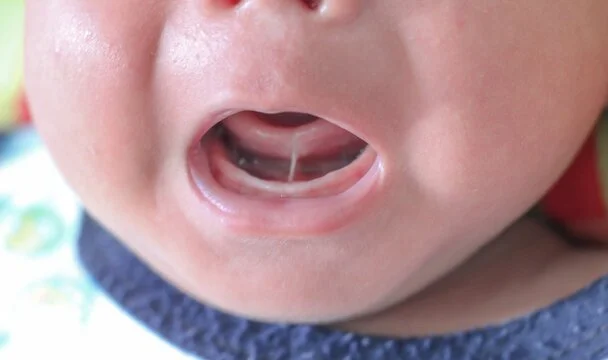
NOTE: it is impossible to diagnose any kind of oral tie just by a visual assessment.
This baby could have a tongue tie, but are there other signs?
Diagnosing a tongue tie should include a thorough assessment:
Visual assessment: looking for oral ties, poor oral alignment, facial asymmetry
Physical assessment: infant suck strength/rhythm, oral restrictions to the tongue/lips/cheeks, body tension
Feeding assessment from beginning to end
Pregnancy, labour and birth, and feeding history
When it comes to any kind of breast/chest feeding challenge, there should be a collaborative team approach. This team could include: your primary care provider, Lactation Consultant, and other health professionals (such as osteopathic manual practitioners, physiotherapists, or chiropractors).
Role of the Lactation Consultant
Working with a Lactation Consultant who has experience supporting babies with a potential tongue tie is important to rule out other potential feeding challenges. As infant feeding specialists, IBCLC’s are trained in supporting human lactation and safe infant feeding practices. There may be other feeding related issues with similar signs and symptoms of a tongue tie. Your IBCLC can also recommend other health care professionals, supports, or strategies to help you reach your feeding goals.
Treatment Options
Not all babies who have oral ties will require a surgical release. If you and your team feel that your baby does have an oral tie, and it is causing feeding challenges, consulting with a provider who can perform a frenotomy should be considered. Frenotomy means to divide the tissue with a surgical cut. A trained doctor or nurse practitioner can use scissors to release these tissues; a Dentist who has specialized training in working with newborns can use a laser.
Potential Risks
A frenotomy is generally a safe and well-tolerated minor surgical procedure, but with any surgical procedure there can be risks.
Some potential risks of a frenotomy: bleeding, nerve injury, infection, pain or oral aversion/breast refusal, reattachment of the tissue, scar tissue, no improvement or change in symptoms or feeding challenges.
It is important to discuss any concerns you have with the healthcare provider.
Preparing for a Frenotomy
Your provider will discuss the procedure with you and the average length of time it will take (from start to baby being back in your arms). Being prepared in advance can provide you with reassurance and help reduce your stress making the overall process as smooth as possible.
If the clinic allows, bring a support person.
You may find it helpful to have another set of eyes and ears for questions and remembering instructions. If you are travelling a far distance, your support person can drive or sit in the back seat with your baby to help keep them occupied.
Ask about pain relief options.
Your milk will help manage your baby’s pain. Spending extra time skin to skin, or baby wearing/carrying, can also help soothe your baby. Your provider may recommend another pain relief option, which you can bring with you to your appointment.
My favourite baby wearing carriers that have been designated “hip-healthy” by the International Hip Dysplasia Institute :
Ergobaby Omni 360 All-Position Baby Carrier for Newborn to Toddler on Amazon.ca
or visit Ergobaby.ca using this link to get 30% off the Embrace Mesh Newborn Carrier
Baby Tula Explore Carrier and use this link to save 20% off your order
Bring your feeding supplies.
After the procedure, your provider will recommend that you feed your baby. If you use any supplies (like a nipple shield, bottles, extra breast milk, formula) make sure you bring them with you. If you are pumping, you may want to bring your pump as well if you are travelling a far distance. Work with your IBCLC beforehand to discuss how to best prepare for feeding your baby following their procedure.
Plan to have no plans.
Your baby may need some extra one-on-one time, and you may notice a change in their feeding and sleep routine for a few days. If possible, try to avoid scheduling any appointments or social visits for a few days.
How your support system can help.
If you have family or friends offering to help, or have “if you need anything let us know!” offers, this is the time to accept. Childcare for older children, preparing meals/snacks, running errands, whatever you feel would be most helpful for you and your baby.
Diagnosing and treating a tongue tie requires a team approach. If you have questions about your feeding journey and your baby, working with an International Board Certified Lactation Consultant is a great first step!
Sweet Pea Lactation Consulting offers virtual consultations globally, and in-home consults in the Annapolis Valley, Nova Scotia.
Resources:
https://www.lllc.ca/tongue-and-lip-ties
https://llli.org/breastfeeding-info/tongue-lip-ties/